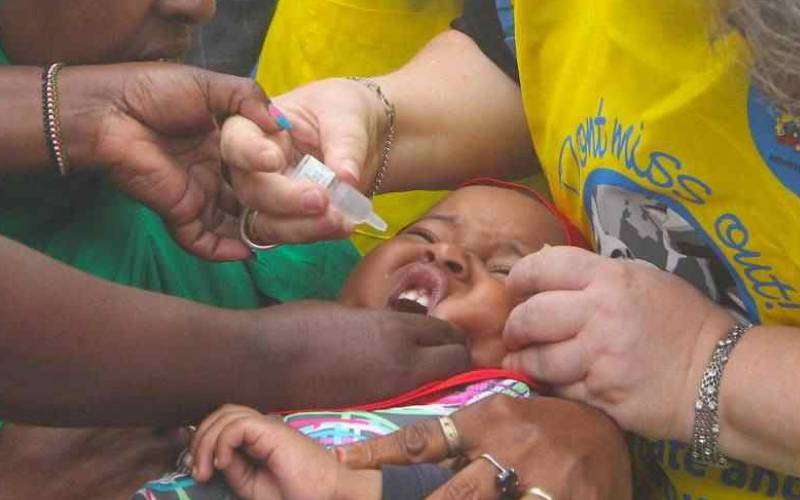
A child receives drops of the polio vaccine in Eastleigh, Nairobi. [File, Standard]
Efforts to improve child immunisation in Kilifi County reveal a deeper struggle between cultural beliefs, access barriers and the capacity of the health system.
At the centre of this transformation are Community Health Promoters (CHPs), who are working to translate national policy into meaningful change at the household level.
In many homes, long-held cultural beliefs still outweigh medical advice. This is especially critical for families with newborns and children under five, an age group for which immunisation is vital for survival.
Yet traditional views in some communities continue to discourage vaccination, exposing children to preventable diseases such as measles and chickenpox and increasing risks of complications or early death.
These tensions are evident within Kilifi County’s primary healthcare system, where immunisation planning, funding and outreach are coordinated through devolved county structures under Kenya’s health governance framework.
For some families, resistance to vaccination is rooted in deep cultural conviction.
Jemima Katana, 76, from Dodosa village and a member of the Mijikenda community, says she raised her children without vaccinations, believing ancestral protection was sufficient.
“My son is named after his great-grandfather, who was a seer. In our culture, we believe he watches over his health,” she says.
Katana also once believed vaccinated children had weaker immunity than those who were not immunised.
That perception began to shift when she met Community Health Promoter Mwanamkasi Hassan during a community outreach session.
Immunisation trends
Mwanamkasi began her work in 2014, moving door-to-door to educate families on the importance of immunising children under five. Through repeated engagement, she encouraged parents to visit health facilities and adhere to vaccination schedules.
“My goal is to ensure no child is left behind. Every child should receive all required vaccinations by 18 months and continue clinic visits until age five,” she says.
According to the Kilifi County 2025 Long Rains Food and Nutrition Security Assessment Report, 76 per cent of children were fully immunised as of June 2024. Measles coverage stood at 76.7 per cent, marking a slight decline compared to the previous year.
Data from a Nutrition SMART survey conducted in June 2023 showed higher coverage earlier, with 89.8 per cent of children aged one receiving basic antigens and measles coverage at 80 per cent.
Consistent engagement
The report attributes the recent decline partly to vaccine stockouts between March and May 2024, which disrupted services and weakened community trust in health systems.
Despite these setbacks, overall progress reflects sustained efforts by healthcare workers and CHPs.
Through consistent engagement, they have worked to dispel myths and challenge long-standing cultural beliefs that previously hindered vaccine uptake.
These efforts align with Kenya’s broader universal immunisation goals under national health policy and devolved healthcare structures, as well as continental commitments to reduce child mortality.
Mwanamkasi serves more than 230 households, making daily visits to ensure children receive vaccinations on schedule. After nearly a decade of outreach, she has witnessed a gradual shift in attitudes.
“I can confidently say cases of whooping cough and curved back have almost disappeared here compared to before,” she says.
She recently trained nursing mother Gladicy Kadzo on child immunisation. Kadzo admits she was once hesitant due to cultural beliefs.
“Back then, I didn’t see the need to vaccinate my child. We believed children were protected by ancestors,” she says. “But my son has already received the measles vaccine.”
Kadzo now encourages stronger government support for CHPs, including allowing them to administer vaccines during home visits, especially in hard-to-reach areas.
“Many children born at home remain undocumented and unvaccinated. When they die, they are buried without ever being recorded in government systems,” Mwanamkasi notes.
Each month, she visits over 80 households and refers sick children to health facilities.
Her work is grounded in prevention and early intervention. She also explains that conditions such as a curved back can be fatal if untreated.
Over time, she has seen growing acceptance of immunisation. “People used to say vaccines have demons. But now even those who missed appointments come asking for them,” she says.
She also participates in community barazas, where health issues are discussed openly. “We now educate communities on timely vaccination through public forums,” she explains.
Beyond immunisation, Mwanamkasi supports child nutrition programmes in collaboration with Kilifi Referral Hospital, distributing vitamin A and deworming medication every six months. She carefully records each child’s treatment to ensure proper follow-up.
She also trains mothers to use Mid-Upper Arm Circumference (MUAC) bracelets to detect malnutrition early. A yellow or red reading signals the need for urgent medical attention.
“I train mothers to screen their children. It is a simple tool that helps prevent severe malnutrition,” she says.
System constraints
Despite progress, challenges remain. The 2025 county report recorded 40 measles cases, with Magarini sub-county accounting for the majority. The under-five mortality rate stands at 0.17 per cent
Nationally, UNICEF reports that fewer than half of Kenyan children receive full doses of both measles and rubella vaccines.
In Kilifi, structural constraints continue to affect coverage. These include delayed funding for CHPs, limited outreach resources and difficult terrain in remote areas.
Mwanamkasi notes that frequent household movement in some areas makes follow-up difficult.
However, she has observed positive change, particularly more facility-based deliveries, which improve early vaccination uptake.
“More mothers now deliver in hospitals, which helps children begin vaccination on time,” she says.
Exclusive breastfeeding rates have also improved, rising to 91.4 per cent from 86.6 per cent in 2022, according to health data.
Before CHPs intensified outreach, many parents only learned about vaccination when children were already sick and taken to the hospital.
To strengthen outreach, Mwanamkasi calls for timely government support and transport facilitation for CHPs.
Under a national stipend programme, CHPs are entitled to a monthly payment shared between the national and county governments.
However, delays in county payments continue to hinder their work.
“The county does not pay us on time. We are owed several months,” she says. “We are doing our part; the government should do its part.”
She recalls a case of a neglected, HIV-positive child she rescued, who later recovered and completed immunisation. “He is now in high school. He calls me his mother,” she says.
Strengthening the system
Kilifi County Health Director Dr Hassan Lela says immunisation coverage has improved, with 60.7 per cent recorded in the last financial year. Outreach programmes and partnerships have helped expand access.
“We are working across all sub-counties to improve coverage and access,” he says.
He stresses the importance of facility-based deliveries and antenatal care in ensuring timely immunisation.
“Mothers must deliver in health facilities so children are fully immunised by age two,” he says.
He also urges vaccination for girls aged 10 through school-based Human Papillomavirus (HPV) programmes to prevent cervical cancer.
Primary Healthcare Coordinator Edward Mumbo says all health centres offer vaccination services, supported by CHPs who conduct mobilisation and follow-up.
However, he notes that funding gaps and long distances remain major barriers. Some residents walk over 10 kilometres to reach health facilities.
He also highlights persistent myths around vaccines, particularly HPV, which have slowed uptake in some areas.
“We are working to change perceptions and improve demand,” he says.
Mumbo calls for stronger collaboration between health workers, teachers and parents to improve school-based vaccination.
“Teachers, parents and health workers must work together,” he says.
Last-mile challenges
While progress is evident, Kilifi’s immunisation drive still faces last-mile challenges. Limited partners, weak funding streams and logistical constraints continue to affect outreach in remote areas.
CHPs remain central to bridging this gap. Their work has improved awareness, strengthened follow-up systems and helped restore trust in immunisation services.
As Kilifi continues to expand its vaccination efforts, the key question remains whether these gains will be sustained through stronger financing, institutional support and accountability, or risk stalling without them.
This story was produced as part of the Seats of Change Fellowship project, a community journalism initiative implemented under the GIZ AU AWARE Programme — AWARE (Promotion of Human Rights and Empowerment of Women in Africa).
 The Standard Group Plc is a multi-media organization with investments in media
platforms spanning newspaper print
operations, television, radio broadcasting, digital and online services. The
Standard Group is recognized as a
leading multi-media house in Kenya with a key influence in matters of national and
international interest.
The Standard Group Plc is a multi-media organization with investments in media
platforms spanning newspaper print
operations, television, radio broadcasting, digital and online services. The
Standard Group is recognized as a
leading multi-media house in Kenya with a key influence in matters of national and
international interest.
