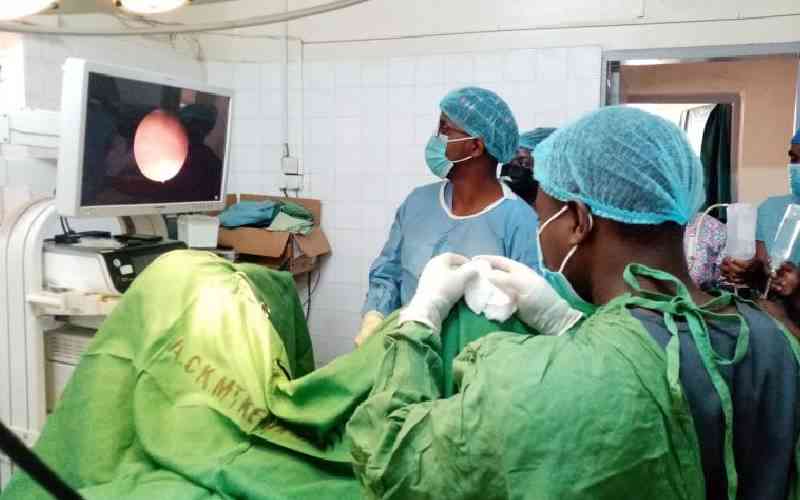
Gynaecological conditions are a major contributor to morbidity and mortality worldwide, with the greatest burden borne by women in resource-limited countries where access to specialised services remains a challenge.
And while great progress has been achieved in reducing maternal mortality worldwide, thanks largely to the Millenium and Sustainable Development Goals (MDG & SDG) initiatives, deaths due to gynaecological conditions such as cervical cancer have continued to rise unchecked, driven largely by a global epidemic of non-communicable diseases (NCDs). Overall, 4.5 per cent of the global burden of disease has gynaecological origins.